|
Age |
Calcium Range (mmol/L) |
|
≤ 27 days |
2.00-2.70 |
|
28 days – 15 years |
2.20-2.70 |
|
≥ 16 years |
2.20-2.60 |
Calcium
Test Alias / Common Abbreviations
Ca, Adjusted calcium, Total calcium
Department
Royal Stoke University Hospital, County Hospital, Leighton Hospital, Macclesfield District General Hospital
Pre-analytical information
Add-on requests: accepted up to 72 hours post sampling
Minimum Retest Interval: not applicable
Sample Collection instructions:
Collect the blood sample using normal venepuncture technique into a serum or lithium-heparin plasma tube (gold/red/green-top).
Sample Transport & Stability Information:
Samples should be sent to the laboratory on the same day as collection to ensure sample integrity is maintained. If a delay in receipt of the sample is anticipated, please contact the laboratory to discuss storage requirements.
Stable in separated serum for 1 day at room temperature and 7 days at 4-8oC.
For generic information on test requesting, sample labelling and packaging, and sample transport – see the frequently asked questions here.
Sample Type, Container & Volume
Adult sample type:
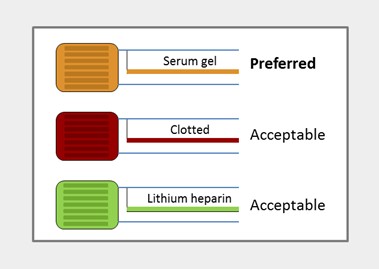
Paediatric sample type:
Lithium-heparin plasma, Plain serum.
Turnaround Time
Based on receipt at testing site.
Within 24 hours.
Calcium is part of the bone profile.
Adjusted calcium is calculated from serum total calcium and albumin concentration. If albumin concentration is <20 g/L or >50 g/L, it is not possible to calculate adjusted calcium. Measurement of ionised calcium, available on POCT blood gas analysers, is a better indication of calcium status at low albumin levels when adjusted calcium is unavailable.
Please note: magnesium is not part of a standard bone profile - please request separately if needed.
Factors that significantly affect result
Contamination with potassium EDTA or trisodium citrate due to poor venesection may artificially lower calcium concentration.
There are a number of non-pathological factors that can influence levels of specific analytes, giving falsely elevated or reduced levels. If you require more information regarding the effects of these factors on the individual test results, please contact the Duty Biochemist.
Serum/plasma samples are routinely screened for the presence of haemolysis, icterus and lipaemia. Results are not reported if one or more of these has been detected at levels deemed to have had a significant impact on the accuracy of the test.
Local guidance documents for investigation of hyper and hypocalcaemia in primary care are available. Please see the following: Adult Hypercalcaemia Primary Care Guidance, Adult Hypocalcaemia Primary Care Guidance.
For more information, please see the following: Calcium
Reviewed / Updated On: 02/12/2025
